Manhattan Diabetic Retinopathy Treatment
Diabetic patients are often at extra risk when it comes to eye problems. Diabetic patients are more likely to develop glaucoma, cataracts, and are also susceptible to diseases such as diabetic macular edema and diabetic retinopathy. People with all types of diabetes (type 1, type 2, and gestational) are at risk for diabetic retinopathy. Risk increases the longer a person has diabetes. 40 to 45 percent of Americans with diabetes have some stage of diabetic retinopathy.
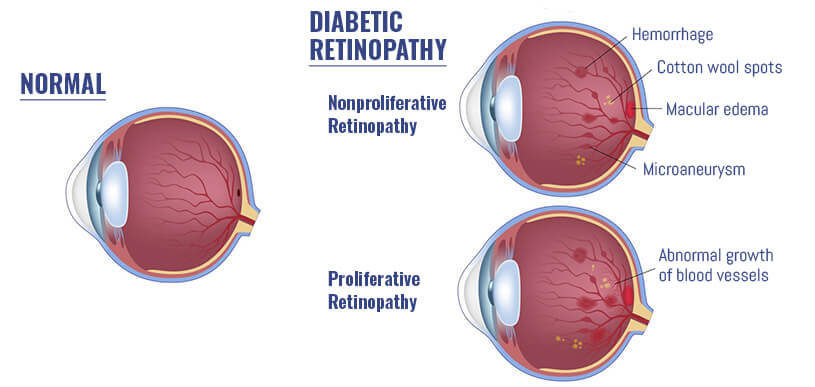
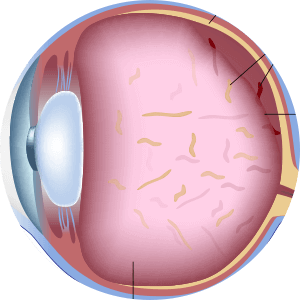
What Causes Diabetic Retinopathy?
Diabetic retinopathy is a condition caused by chronically high blood sugar. This damages the tiny blood vessels in the retina. The retina detects light and converts it to signals sent through the optic nerve to the brain. Diabetic retinopathy causes tiny blood vessels in the retina to leak fluid or bleed, distorting vision. In the most advanced stage of diabetic retinopathy, new abnormal blood vessels begin to grow on the surface of the retina, which can lead to scarring and cell loss in the retina.
Is Diabetic Retinopathy Preventable?
Diabetic retinopathy is preventable with good blood sugar control. Vision lost to diabetic retinopathy is irreversible, but early detection and treatment can reduce the risk of blindness by 95 percent. Because there are often no symptoms in the early stages of diabetic retinopathy, patients with diabetes should have an eye exam every year, where the eye doctor will screen for diabetic retinopathy. This is the only way to diagnose diabetic retinopathy and catch it in its early stages. Some studies show that controlling diabetes slows the worsening of diabetic retinopathy.

What it’s like to see with diabetic retinopathy
How is Diabetic Retinopathy Treated?
Diabetic Retinopathy is not curable, but it can be treated to slow progression. Laser treatment is often used to treat diabetic retinopathy. The laser beam can used to create small burns in areas of the retina with abnormal blood vessels to seal the leaks. Treatment depends on the stage of the disease and is directed at trying to slow or stop progression.